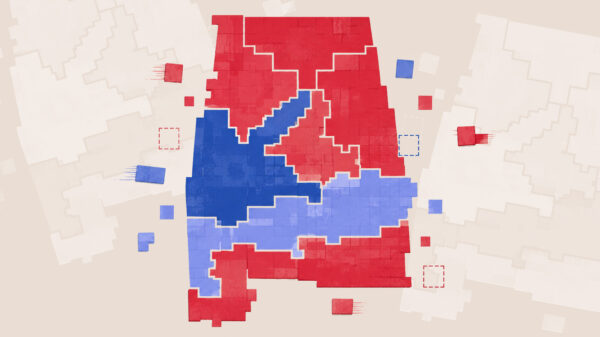
Alabama’s seven-day average positivity rate — the percent of COVID tests that came back positive — reached a record-high 27 percent on Wednesday, according to the Alabama Department of Public Health, and hospitalizations are increasing rapidly as well, as the more contagious omicron variant continues surging in the U.S.
Dr. Bobby Lewis, vice chair of clinical operations for UAB’s Department of Emergency Medicine, told reporters during a Wednesday briefing that every emergency department in Birmingham has been seeing record numbers of patients, and COVID is the driving force.
All three of the emergency rooms operated by UAB on a busy day would see about 450 patients, but on Tuesday saw 617 patients, Lewis said.
“We’re not to the point of having to call in the National Guard or other things that some other states have seen, but if the rise keeps going that may be a possibility We don’t know when this is going to peak,” Lewis said, explaining that UAB is gearing up staffing and resources to ensure readiness if hospitalizations increase due to gatherings New Years eve.
“One way or another we’ll make everything happen, but it certainly is getting to a critical point,” Lewis said.
{{CODE1}}
{{CODE2}}
COVID hospitalizations in Alabama on Wednesday reached 720, according to ADPH, which was an 89 percent increase over two weeks. All but one Alabama county is deemed to have high levels of community transmission, according to the department.
Alabama’s ICU beds statewide were at 86.3 percent capacity on Wednesday, with 11.7 percent being taken up by COVID patients, according to the U.S. Department of Health and Human Services
Alabama’s seven-day average of new daily cases reported to the Alabama Department of Public Health broke 2,000 on Monday for the first time since Sept. 29, reaching 2,100. Nearly 6,000 newly reported cases were added to the state’s official tally on Wednesday.
{{CODE3}}
Lewis said that fortunately the omicron variant doesn’t tend to produce as severe an illness in most people, but the sheer number of infections is driving hospitalizations.
“This huge number of people that are getting infected is what’s really causing this surge that we’re seeing,” Lewis said. “These numbers are much greater than we saw in the previous surge that we had, and we were ill-prepared to take care of those when it first started. Now we’re much better prepared, but we’re seeing greater numbers.”
Lewis said approximately 97 percent of those being hospitalized with COVID are unvaccinated.
Lewis cautioned the public not to show up at emergency rooms if they have mild symptoms and are seeking a COVID test, explaining that emergency room care is best suited for those with more severe COVID symptoms, including shortness of breath, fever, and persistent cough.
“Those things are generally better taken care of at a primary care doctor’s office or in a clinic, or in one of the freestanding emergency departments,” Lewis said of COVID testing.
For those unsure of where to get a COVID test, Lewis encouraged them to call a hospital to receive information on the best testing location for them.