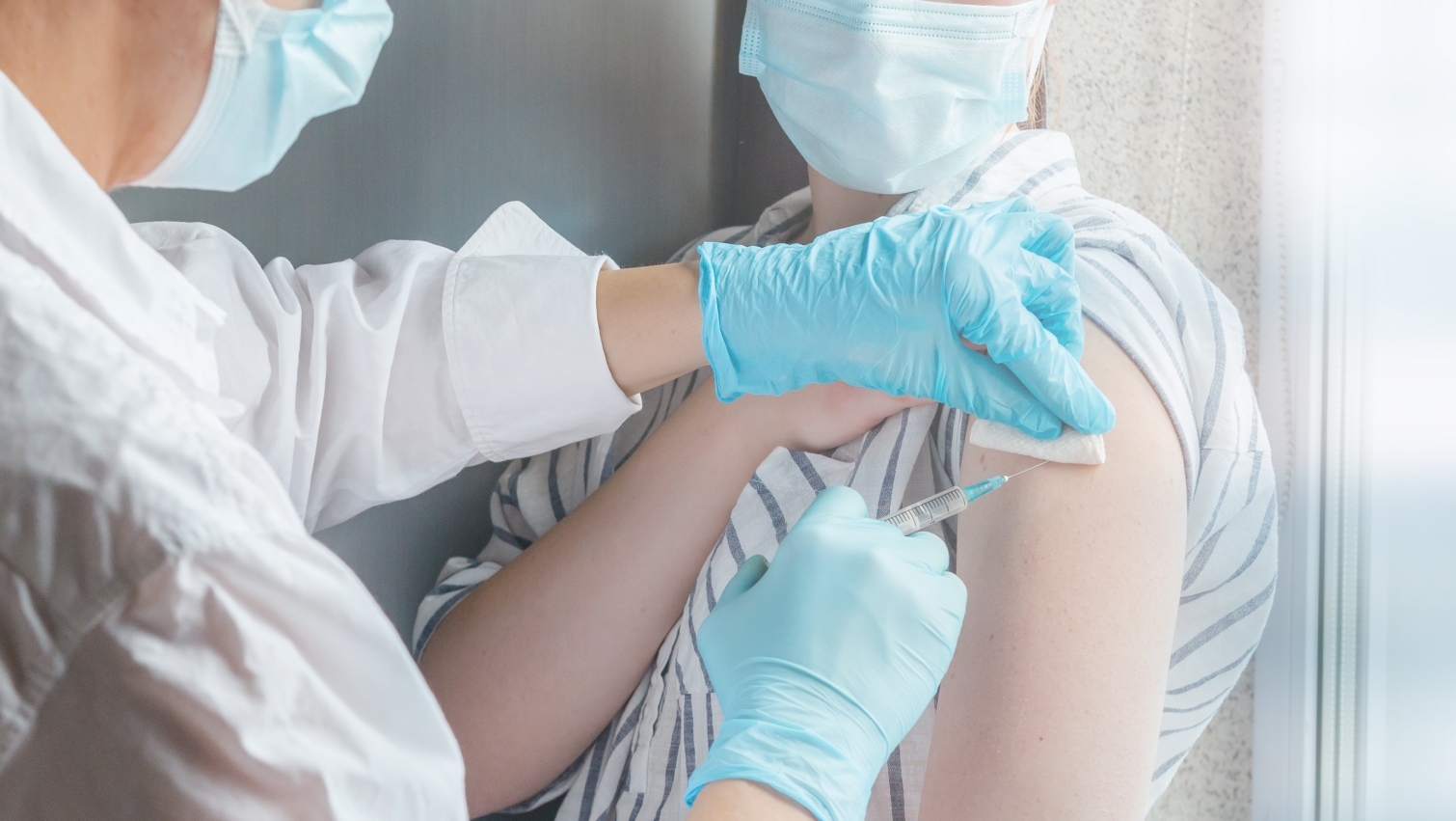
COVID-19 cases and hospitalizations in Alabama are surging. What’s clear, however, is that the vaccinated aren’t getting as sick as the unvaccinated, explained UAB Hospital’s infectious disease director.
UAB’s Dr. Jeanne Marrazzo is also the treasurer of the Infectious Diseases Society of America’s board of directors, and during an IDSA briefing on COVID Tuesday, Marrazzo explained that it’s clear by looking at who’s hospitalized with COVID, who’s in ICU’s and on ventilators, that COVID vaccines are working.
Marrazzo said at UAB Hospital “the vast majority overwhelmingly are unvaccinated people in all categories.”
At UAB on Tuesday 70 percent of the 193 hospitalized with COVID were unvaccinated, 75 percent of those patients in the hospital’s ICU were unvaccinated and 73 percent of the 30 patients hooked to ventilators were unvaccinated.
Statewide COVID hospitalizations have more than doubled over the last two weeks, reaching 1,925 on Tuesday, according to the Alabama Department of Public Health.
{{CODE1}}
Alabama’s average daily COVID cases reported to the Alabama Department of Public Health over the week ending Monday broke 10,000 for the first time ever, reaching 10,047.
{{CODE2}}
The state’s seven-day average of daily percent positivity, or the percent of COVID tests that are positive, was 41.2 percent on Tuesday. Public health experts say it should be at or below five percent or cases are going undetected.
{{CODE3}}
All of Alabama’s 67 counties are classified by the Alabama Department of Public Health as having high levels of community transmission
Marrazzo also discussed the current lack of the availability of effective COVID treatments and the rash of hospital staff who have either tested positive or COVID, requiring isolation, or been exposed, requiring quarantining.
“We have limited access to monoclonal antibodies that work. In fact, we have none right now. We’re waiting on a shipment,” Marrazzo said. “We don’t have the oral drugs yet, and we don’t have any other options.”
The federal government on Dec. 24 temporarily paused shipments to states of two monoclonal antibody treatments, made by Eli Lilly and Regeneron, after it became clear the two treatments were ineffective against omicron.
One other monoclonal antibody treatment that is effective against omicron, called Sotrovimab, is in short supply nationwide as the shrug-maker ramps up production. Shipments of the other two antibody treatments resumed in January, but hospitals that had operated monoclonal antibody treatment centers, including UAB, were still recently debating how to move forward.
Another new COVID treatment available to medical providers, Pfizer’s antiviral pill Paxlovid, is also in short supply. In Alabama, the drug is being allocated to Walmart stores, requires a doctor’s prescription to obtain and is saved for only those at greatest risk of serious complications due to COVID. Paxlovid can cut the need to hospitalize someone with COVID by 88 percent if taken within the first few days of contracting the virus. The U.S. Food and Drug Administration approved emergency use for Paxlovid and another antiviral pill, molnupiravir, just before Christmas.
In addition to getting vaccinated and booster shots, one thing the public can do is to continue doing what is know to work, which is to wear face masks, Marrazzo explained.
“We’ve known this from the beginning. Lots and lots of data at the community level, even at the country level in some places. Masks really work,” Marrazzo said. She also discussed the question of whether to trade in cloth masks for N95 or KN95 masks, which provide better protection from the virus.
“If you can get them and you can wear them, and they’re comfortable enough for you to wear them in the settings you need them, absolutely,” Marrazzo said of the N95 and KN95 masks.
The fit of the N95 or KN95 needs to be correct around the face to provide the best protection, Marrazzo explained, noting that there are cloth masks that fit very well, and the most important thing is that people wear masks when needed. Masks are recommended especially when indoors around others, in large crowds and where ventilation is inadequate.
“I’m fine with the idea of saying the best thing you can do is wearing an N95 or a KN95, but the reality is that that’s neither attainable nor comfortable for many people,” Marrazzo said. “And I would much rather see people wear something that they feel is a great fit, really comfortable, particularly if they have to be wearing it eight hours a day standing behind the counter for example, serving people.”